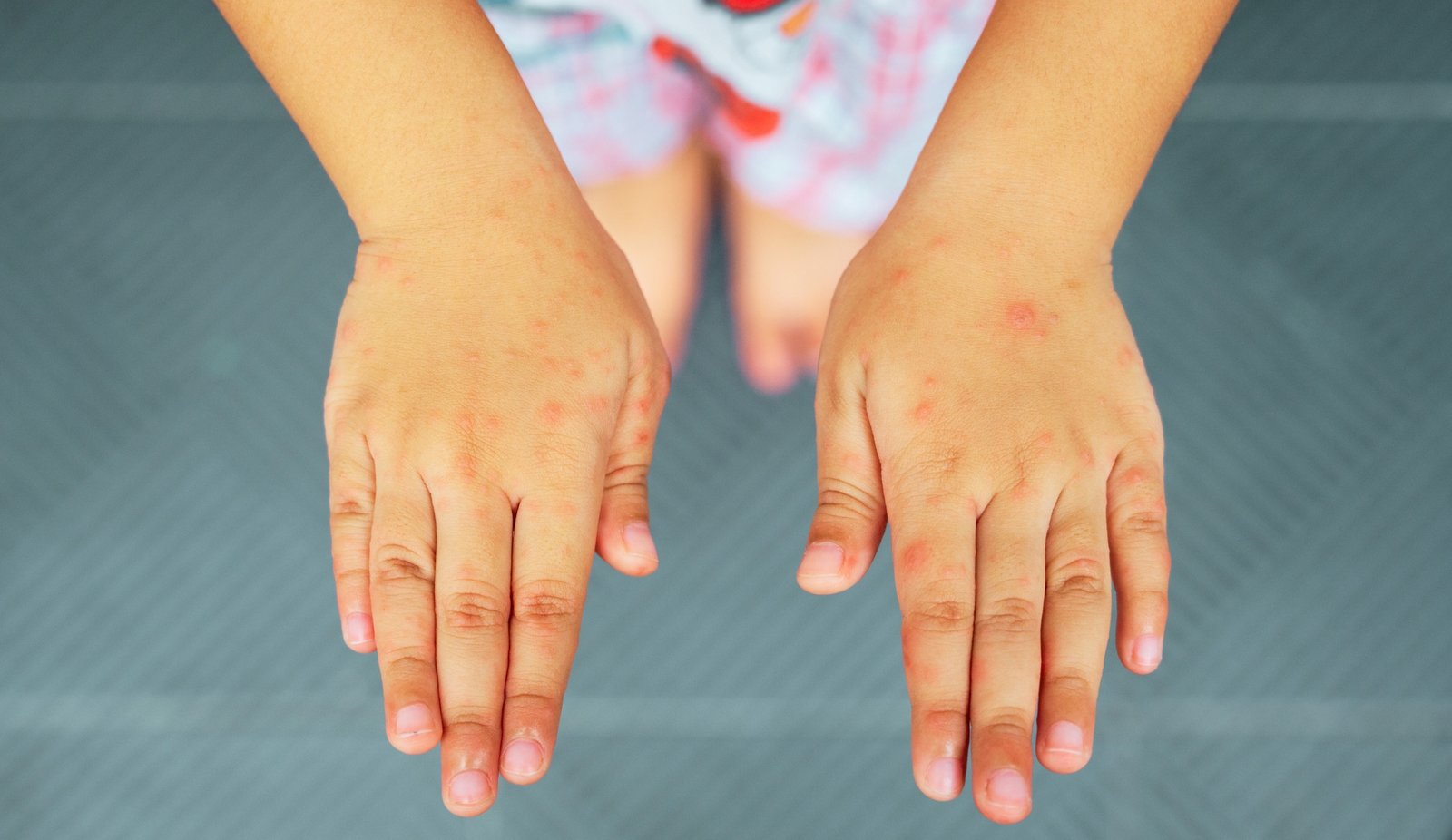
Can adults get Hand Foot and Mouth Disease, or is it something that only affects children? Many people think this illness is exclusive to toddlers, but surprising cases among adults are becoming more common. How does it spread to adults, and what makes their symptoms different from those seen in kids?
Adults can also get Hand Foot and Mouth Disease, though it’s less frequent. Adults with weaker immune systems or close contact with infected children are more likely to contract it. In this article, we’ll break down the symptoms, causes, and recovery process for adults, with expert input from infectious disease specialists.
But here’s where it gets interesting — adult cases often go unnoticed or are mistaken for other viral infections. Dr. John Williams, a leading pediatric infectious disease expert at UPMC, explains that adults may experience milder yet still contagious symptoms.
So, stay with us as we uncover how adults can protect themselves, recognize early signs, and recover faster from Hand Foot and Mouth Disease.
Can Adults Get Hand Foot and Mouth Disease from Children?
Yes—adults can contract hand, foot and mouth disease (HFMD) from children. In many cases, children act as a reservoir for the viruses that cause HFMD, and adults living with or caring for young children may be exposed through close contact.
Here’s how it often happens in practical terms:
- A child in daycare or preschool becomes infected with an enterovirus (often *Coxsackievirus A16 or *Coxsackievirus A6).
- That child has a mild fever, mouth sores, and/or rashes on the hands or feet, and spreads viral particles via saliva, nasal secretions, or stool.
- An adult in the household shares items (toys, cups), touches surfaces (toy bins, door handles) or cleans up after the child—for example, wiping a running nose or changing diapers—and comes into contact with the virus.
- The adult then becomes infected, possibly with fewer or milder symptoms than children. According to one source, “parents can get hand, foot, and mouth disease from their kids, especially if they’re sharing food or drink.”
- Because adults might not realize they’re infected (or may have only mild symptoms), they can inadvertently pass the virus on to others—especially young children or immunocompromised individuals.
Key takeaway: If any child in your home has HFMD, it’s entirely realistic for an adult to pick it up. Good hygiene, surface disinfection, and avoiding sharing drinks/utensils can reduce risk significantly.
Is It Rare for Adults to Get Hand, Foot, and Mouth?
Yes—it is relatively rare for adults to show notable symptoms of HFMD, though infection can occur. The lower incidence in adults is likely due to immunity acquired in childhood (many adults have had sub-clinical or mild infections earlier).
Some stats and observations:
- While children under 5 account for the vast majority of HFMD cases, there are documented case-reports of adults diagnosed with the disease.
- According to one review: “[A]typical presentation may be characterised … in adults … clinical manifestations in less than 1% of adults.”
- Among those adults who are symptomatic, the illness may present atypically (for example more widespread rash, or fewer classic lesions).
- Some adults may be infected yet symptom-free—so prevalence may be higher than the diagnosed numbers suggest.
- The severity of symptoms is usually milder in adults compared to children, but it can vary.
So while not common, adult infection is not impossible, and the “rarity” is mostly a matter of symptomatic detection rather than absolute immunity.
How Can Adults Get Hand and Foot and Mouth Disease?
Let’s get into the transmission mechanics and risk situations for adults. Essentially, the same pathways that allow children to catch HFMD also apply to adults, but with some caveats:
Transmission pathways
- Via respiratory droplets: coughs or sneezes from an infected person can spread the virus. Cleveland Clinic+1
- Via direct contact: touching contaminated surfaces (doorknobs, toys, shared utensils) or caring for someone who is infected. Mayo Clinic+1
- Via the fecal-oral route: viruses may shed in stool for days/weeks, meaning diaper changes, toileting hygiene, and hand-washing are key. PMC+1
Why it happens in adults
- Adults may lack immunity to the exact viral strain the child has (for example a newer variant), so prior childhood exposure doesn’t guarantee protection. Duke Health+1
- Close contact with children (parents, childcare workers) increases exposure risk.
- Shared environments—daycares, schools, playgrounds—can lead to spread into the adult household.
- Adults with weakened immune systems may be more likely to become symptomatic if infected. Cleveland Clinic+1
Risk factors to watch
- Caring for children with HFMD (especially diaper age)
- Inadequate hand-washing after child care/diaper changes
- Sharing items or close face-to-face contact with infected child
- Immunocompromised condition, pregnancy, or underlying illness (increasing risk of more severe presentation) Cleveland Clinic
In summary: Adults ‘get’ HFMD when exposed, especially via children, and prevention depends heavily on hygiene and limiting exposure to infected secretions or surfaces.
Symptoms of HFMD in Adults vs. Children
Understanding how symptoms differ between adults and children helps with recognition, diagnosis, and appropriate care.
Common symptoms in children
- Fever, sore throat, loss of appetite, sometimes runny nose.
- One to two days later: painful mouth sores (vesicles or ulcers on tongue, gums, inside cheeks).
- Rash on palms, soles, sometimes buttocks and legs; may turn into blisters; rarely very itchy.
Symptoms in adults
Adults may present with similar features, but with some differences:
- Fever and sore throat – yes, but sometimes milder or shorter duration.
- Mouth sores – yes, but could be less obvious or mistaken for other causes.
- Rash/blisters – may occur but less consistently; distribution may include trunk, arms, buttocks, not just hands/feet.
- Possible malaise, fatigue, muscle aches—these might appear stronger than expected.
- Some adults may be asymptomatic carriers (i.e., infection with no overt signs).
Here’s a quick comparison:
| Feature | Children | Adults |
|---|---|---|
| Fever & sore throat | Common | Often milder or absent |
| Mouth sores | Clear, painful | Possibly milder or less obvious |
| Rash/blisters on hands/feet | Typical | Less predictable, may involve other areas |
| Asymptomatic cases | Less common | More common |
| Duration of symptoms | ~7-10 days | Can be similar, sometimes longer |
Because adult cases are often milder or atypical, they may go undiagnosed or be mistaken for other viral illnesses.
What Does Hand Foot and Mouth Disease Look Like on Adults?
Visual recognition is helpful, especially for adults who may be trying to decide whether to seek medical attention or isolate. The typical signs in adults when symptomatic include:
- Small red spots or bumps on palms and soles, which may blister into classic fluid-filled lesions.
- Mouth ulcers on tongue, gums, inner cheek, or throat; these can be quite painful and may interfere with eating/drinking.
- Rash or blisters possibly extending beyond hands and feet—arms, legs, buttocks, and even torso in some cases.
- In some adult cases, the rash may be faint, or the spots may be mistaken for other skin conditions.
Because adult presentation can be varied, here are a few watch-points:
- If you notice unexplained mouth ulcers plus rash on palms/soles, consider HFMD.
- If you recently had exposure (child with HFMD, daycare setting) and now have vague viral symptoms + rash, HFMD should be in the differential.
- If you are pregnant, have underlying immune-compromise or severe malaise, ask your provider whether HFMD is a possibility.
While I can’t embed images here, you’ll commonly find photos showing blister-like lesions on adult hands or feet, and ulcers on the tongue or gums if you search reputable medical visuals.
How Do You Treat Hand Foot Mouth Disease in Adults?
In adults, treatment of HFMD is largely supportive—because, as with children, there’s no specific antiviral therapy routinely used for this condition. The goal is symptom relief, hydration, and prevention of spread.
What you can do at home
- Manage fever or pain with over-the-counter medications such as acetaminophen (paracetamol) or ibuprofen (unless contraindicated).
- Encourage hydration: mouth sores may make swallowing uncomfortable, so cool liquids, popsicles, or soft foods may help.
- Topical oral pain relief (e.g., soothing mouth rinses, avoiding spicy or acidic foods) supports comfort.
- Keep skin lesions clean and dry; avoid scratching; wash hands thoroughly after contact with blisters or secretions.
- Isolate from others (especially young children or immunocompromised) while symptomatic to reduce spread. According to one article, “you should stay home … because the disease is contagious.”
When to seek medical attention
Although most adult cases are mild, certain situations warrant seeing a healthcare provider:
- Difficulty swallowing, severe mouth ulcers, inability to drink fluids (risk of dehydration)
- Significant rash or blistering beyond typical locations (hands/feet)
- Underlying immune-compromise or pregnancy (potential higher risk of complication)
- Symptoms lasting more than 10-14 days or worsening rather than improving
- Signs of complications (for example headache + stiff neck raising concern for meningitis, though very rare)
Duration and outlook
- Most adults recover in about 7-10 days once symptoms develop.
- Blisters may take longer to heal, and viral shedding (i.e., ability to infect others) may continue for days or even weeks after symptoms resolve.
- Complications in healthy adults are uncommon—but awareness is key.
In essence: treat symptoms, stay hydrated, prevent spread, and watch for signs of complications.
Should Adults Stay Home If Kids Have Hand, Foot, and Mouth?
This is a critical public health and ethical question. The standard guidance is that an infected person is most contagious during the first week of illness. However, the virus can remain in stool for several weeks.
For adults who contract HFMD, the recommendation is clear: Yes, you should stay home. You are contagious and can spread the virus to coworkers, friends, and the public. Stay home until your fever has resolved for 24 hours (without fever-reducing medication) and the blisters have begun to heal and crust over. This typically means at least a few days to a week away from work.
For adults who are exposed but not yet sick, the situation is more nuanced. You are not required to isolate preemptively. However, you should be hyper-vigilant about hygiene and monitor yourself closely for symptoms.
If you work in a high-risk environment (e.g., a healthcare setting, daycare, or with immunocompromised individuals), it is prudent to inform your employer and discuss a potential contingency plan. The key is to practice scrupulous hygiene to avoid becoming a vector for the disease in your community.
Commonly ASked Questions about How Can Adult Get HFMD (FAQs)
Can adults get hand foot and mouth disease?
Yes, adults can get hand foot, mouth disease (HFMD), although it is more common in children, especially those younger than 5 years. The disease is caused by a contagious viral infection and can lead to painful sores in the mouth and a skin rash.
What are the symptoms of hand foot and mouth disease in adults?
Symptoms of hand foot and mouth disease in adults can include mouth sores, throat pain, fever, and skin rash. Adults may not experience symptoms as severely as children, but they can still develop painful sores in their mouth and discomfort.
How is hand foot and mouth disease contagious?
HFMD is highly contagious and spreads through close contact with an infected person, oral secretions, or surfaces contaminated with the virus. Adults can easily contract the virus from children, especially in settings like daycare centers or schools.
What should I know about hand foot and mouth disease treatment?
There is no specific treatment for HFMD, but most symptoms usually resolve on their own within 7 to 10 days. Treatment for HFMD primarily focuses on relieving symptoms, such as using over-the-counter pain relievers and staying hydrated.
Can adults experience severe symptoms from hand foot and mouth disease?
While adults can get HFMD, they usually experience milder symptoms compared to children. Severe symptoms are uncommon in adults, but they can occur, especially in those with weakened immune systems.
How long are adults contagious with hand foot and mouth disease?
Adults are contagious during the time they exhibit symptoms and can continue to spread the virus for several days after symptoms go away. It’s essential to maintain good hygiene to prevent further transmission.
What steps can be taken to relieve symptoms of hand foot and mouth disease?
To relieve symptoms, adults can take over-the-counter medications for pain relief, drink plenty of fluids, and avoid spicy or acidic foods that may aggravate mouth sores. Good oral hygiene can also help in managing symptoms.
What are the differences in HFMD symptoms between children and adults?
HFMD symptoms can vary between children and adults. Children often show more severe symptoms, including a higher incidence of mouth sores and skin rashes. Adults may experience throat or mouth pain but often have milder or fewer symptoms overall.
Conclusion
In sum, while hand, foot and mouth disease is most commonly seen in young children, the question “can adult get hfmd” must be answered with a clear “yes.” Adults can and do become infected—although they are less likely to display classic, full-blown symptoms. Because adult cases are often milder, they can go unrecognized and, in turn, propagate onward to others (including children or immuno-vulnerable persons).
Understanding how adults catch the disease (often via close contact with infected children), recognizing how symptoms may differ from childhood cases, and knowing what to do if you become infected will help you respond proactively. Good hygiene, hygiene-conscious behaviour, and prompt symptomatic care are the cornerstones of effective management. If you are ever in doubt about symptoms, especially if you are pregnant or immune-compromised, speak with a healthcare provider. By staying informed and vigilant, adults can protect themselves — and by extension, the children and community around them.
Recommended posts
- The 3 Stages of Hand Foot and Mouth Disease (A Complete Guide)
- 7 Best Natural Remedies for Hand Foot and Mouth Disease
- The Alarming Rise of Foot and Mouth Disease in Adults!
- What Causes Hand Foot and Mouth Disease (Must-Read)
- Can 4 Year Olds Get Hand Foot and Mouth Disease (Key Facts)