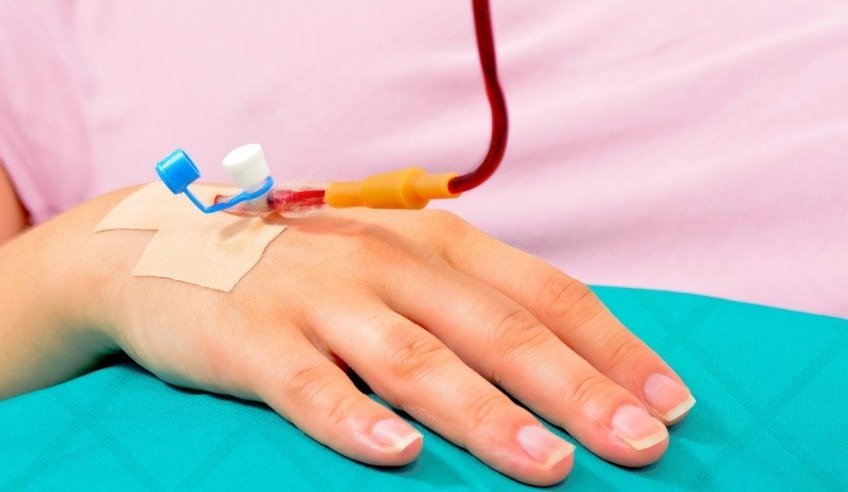
Are you worried about anemia during pregnancy and considering an iron transfusion? Is iron transfusion while pregnant safe for you and your baby? Understanding the benefits and risks can help you make the right choice for a healthy pregnancy.
Iron infusions during pregnancy are generally safe when administered under medical supervision and are recommended for women with severe anemia or when oral iron fails. According to Dr. Sarah Kilpatrick, a leading obstetrician, these transfusions quickly restore hemoglobin levels and reduce risks like fatigue, preterm labor, and low birth weight. With proper monitoring, most women tolerate the procedure well.
But safety depends on timing, dosage, and individual health conditions. From possible mild side effects to important precautions, knowing what to expect can ease your concerns. Let’s dive into the details of iron transfusion during pregnancy and how it can support both mother and baby safely.
Is Treatment Available for Anemia or Iron Deficiency During Pregnancy?
Absolutely, yes. Treatment for anemia and iron deficiency during pregnancy is not only available but is a standard and crucial component of prenatal care. The approach to treatment is typically tiered, escalating in intensity based on the severity of the deficiency, your body’s response, and your overall health.
The first line of defense is almost always oral iron supplementation. Your obstetrician will likely recommend a daily prenatal vitamin containing iron and may prescribe an additional separate iron supplement if blood tests indicate your levels are low.
This method is effective for many women, but it has significant limitations. Oral iron is notorious for causing gastrointestinal side effects like constipation, nausea, and stomach cramps, which can be particularly challenging to manage during pregnancy.
Furthermore, the absorption of oral iron can be slow and inefficient, especially if taken with certain foods or medications.
This is where intravenous (IV) iron infusion becomes a critical and available treatment option. It is typically recommended in specific scenarios, including:
- Severe Iron Deficiency Anemia: When your hemoglobin levels drop below a specific threshold (often around 10-11 g/dL, depending on the trimester), and oral supplements are insufficient to correct it.
- Intolerance to Oral Iron: If the side effects of oral iron supplements are so severe that you cannot tolerate taking them consistently.
- Malabsorption Conditions: For women with underlying gastrointestinal issues like Inflammatory Bowel Disease (IBD), Celiac Disease, or those who have had gastric bypass surgery, where the gut cannot properly absorb oral iron.
- Late-Pregnancy Diagnosis: When anemia is diagnosed in the third trimester, and there is insufficient time for oral iron to raise levels adequately before delivery.
- Patient Preference: In some cases, after discussing the options, a patient may opt for the faster, more direct route of an infusion to quickly resolve debilitating symptoms like extreme fatigue.
What Are Iron Infusions in Pregnancy?
An iron infusion is a medical procedure where iron is delivered directly into your bloodstream through an intravenous line. Think of it as a “direct delivery service” bypassing the digestive system entirely.
This method allows for a complete therapeutic dose of iron to be administered in a controlled setting, replenishing your body’s iron stores much more rapidly and efficiently than oral supplements ever could.
The process itself is straightforward and is usually performed in a hospital outpatient clinic, a specialized infusion center, or sometimes in your obstetrician’s office. Here is a step-by-step breakdown of what you can expect:
- Pre-Infusion Assessment: Before scheduling the infusion, your doctor will conduct a thorough evaluation. This includes reviewing your complete blood count (CBC), iron studies (ferritin, transferrin saturation), and your overall medical and obstetric history to ensure you are a suitable candidate.
- The Day of the Procedure: You will be seated in a comfortable chair. A nurse or a trained clinician will insert a small cannula (a thin, flexible tube) into a vein in your hand or arm. Your vital signs, such as blood pressure and heart rate, will be monitored before, during, and after the infusion.
- The “Test Dose”: For certain types of IV iron, the clinician may start by administering a very small test dose over several minutes to observe for any immediate adverse reactions.
- The Main Infusion: If the test dose is well-tolerated, the remainder of the iron preparation will be infused. The duration of the infusion can vary from 15 to 30 minutes for newer formulations (like ferric derisomaltose or ferric carboxymaltose) to several hours for older types. The total dose required is calculated based on your body weight and the severity of your anemia; some women require only one iron infusion, while others might need two, spaced a few days apart.
- Post-Infusion Monitoring: After the infusion is complete, you will be monitored for a short period (typically 30-60 minutes) to ensure you have no delayed reaction. Once cleared, you are free to go home.
How Effective Are Intravenous Iron Infusions During Pregnancy?
The effectiveness of intravenous iron infusions during pregnancy is not just significant; it is often dramatic. Clinical studies and real-world practice consistently demonstrate its superiority over oral iron in rapidly and reliably correcting iron deficiency anemia in pregnant women.
The primary benefits and evidence of its effectiveness include:
- Rapid Hemoglobin Increase: IV iron leads to a much faster rise in hemoglobin levels compared to oral iron. Patients often see a substantial improvement in their blood counts within 2 to 3 weeks, whereas oral iron can take months.
- Replenishment of Iron Stores: Beyond just hemoglobin, IV iron effectively rebuilds your body’s ferritin reserves—the stored iron that acts as a crucial reservoir for you and your baby throughout the remainder of the pregnancy.
- Symptom Resolution: The most noticeable effect for many women is the rapid alleviation of debilitating anemia symptoms. Profound fatigue, weakness, heart palpitations, shortness of breath, and pale skin often improve markedly within the first few weeks post-infusion.
- Improved Maternal and Fetal Outcomes: By effectively treating severe anemia, IV iron infusion reduces the risks associated with the condition, such as preterm birth, low birth weight, and the need for blood transfusions during or after delivery. It also improves maternal well-being and functional capacity, which is invaluable during the demanding final stages of pregnancy and the postpartum period.
Are intravenous iron infusions Safe During Pregnancy?
Can you have an iron transfusion when pregnant? This is the most crucial question for any expectant mother, and the answer, supported by a growing body of robust research, is a resounding yes, they are considered safe when administered under appropriate medical supervision.
The safety profile of modern IV iron preparations is excellent, especially when compared to the risks of leaving severe anemia untreated. However, as with any medical procedure, it is essential to be aware of both the common reactions and the rare risks.
Common, Mild Side Effects:
These are usually temporary and not a cause for alarm. They include:
- A temporary metallic taste in the mouth.
- Minor headaches or dizziness.
- Flushing or a feeling of warmth.
- Mild nausea.
Localized irritation, bruising, or phlebitis (inflammation of the vein) at the injection site. A technique like using a warm pack can help mitigate this.
Serious Risks (Very Rare):
The most significant risk associated with IV iron is an allergic or hypersensitivity reaction, which can range from mild to severe (anaphylaxis). However, it is critical to understand that the incidence of severe reactions has plummeted with the development of newer, more stable iron carbohydrate complexes.
The risk is now estimated to be very low (less than 1%). This is why the procedure is conducted in a controlled medical setting with staff trained to recognize and manage any potential reaction immediately. Your healthcare team will have emergency medications like antihistamines, corticosteroids, and epinephrine on hand.
Weighing the Risks vs. Benefits:
It is vital to contextualize these risks. Untreated severe iron deficiency anemia poses a far greater and more probable threat to both mother and baby than the rare risk of a reaction from an iron infusion. The benefits of restoring your iron levels—increased energy, reduced risk of complications, and better overall health for you and your baby—overwhelmingly outweigh the potential risks for the vast majority of women who require this treatment.
Common Questions about Iron Transfusion While Pregnant (FAQs)
How much iron do pregnant people need?
Pregnant individuals need 27 mg of iron daily. If oral supplements fail or for severe deficiency, a doctor may administer iron intravenously. A single iron infusion can rapidly restore levels, but this requires medical supervision.
When would an IV iron infusion not be advised?
IV iron is not advised for women with iron deficiency who are not anaemic, have a history of anaphylaxis to IV iron, or have an active, untreated infection. Oral supplementation is the first-line treatment.
What are the symptoms of low iron in pregnancy?
Symptoms include extreme fatigue, pale skin, dizziness, and shortness of breath. This occurs because red blood cells cannot carry oxygen effectively, defining anemia in pregnancy. A blood test confirms the diagnosis.
What is an iron infusion and when is it needed during pregnancy?
An iron infusion is a medical procedure where iron is delivered intravenously to increase iron levels in the body. It is often needed during pregnancy when women are diagnosed with iron-deficiency anemia, particularly if oral iron supplements are ineffective or cause gastrointestinal side effects. This is crucial for maintaining healthy hemoglobin levels, especially during the first and third trimesters of pregnancy.
How long does an iron infusion take?
The duration of an iron infusion can take anywhere from 15 minutes to several hours, depending on the specific formulation used and the individual’s needs. Healthcare providers will monitor the patient throughout the procedure to ensure safety and effectiveness.
What are the side effects of iron infusions during pregnancy?
While generally safe, Iron infusions when pregnant can cause side effects such as allergic reactions, discomfort at the injection site, or transient changes in blood pressure. Most side effects are mild and temporary. It’s important for pregnant women to discuss potential side effects with their healthcare provider prior to receiving an infusion.
Can I take oral iron supplements instead of getting an iron infusion?
Many women may prefer to take oral iron supplements to increase iron levels. However, if the anemia is severe or if gastrointestinal side effects prevent proper absorption, intravenous iron may be a more effective treatment option. Consulting with a healthcare provider will help determine the best approach for each individual.
Is iron infusion safe during the first trimester of pregnancy?
Iron infusions can be administered during the first trimester if necessary, particularly for women with diagnosed iron deficiency anemia. Healthcare providers weigh the benefits against any potential risks of iron blood transfusion while pregnant, ensuring that the health of both the mother and fetus are prioritized.
What are the recommended iron levels for pregnant women?
The World Health Organization recommends that pregnant women maintain sufficient iron levels to prevent anemia, typically aiming for a hemoglobin level of at least 11 g/dL. Individual needs may vary, so it’s crucial to consult with a healthcare provider to determine the appropriate course of treatment for each woman’s unique situation.
Conclusion
Can you get iron transfusion while pregnant? Navigating a diagnosis of severe iron deficiency anemia during pregnancy can feel daunting, but it’s important to remember that it is a highly treatable condition. While oral supplements are the first step, an iron transfusion while pregnant is a safe, highly effective, and often life-changing intervention for those who need it. It offers a rapid pathway to replenishing iron stores, alleviating debilitating symptoms, and mitigating the risks associated with anemia for both mother and child.
If you are experiencing severe fatigue and other signs of anemia, have a candid conversation with your obstetrician. Through proper diagnosis and a collaborative discussion about your treatment options, including IV iron infusion, you can confidently take the steps needed to ensure a healthier, more vibrant pregnancy journey.
Recommended posts
- What to Drink to Increase Hemoglobin? (Iron Rich Drinks List)
- Ferritin Levels in Pregnancy Chart (Trimester-By-Trimester)
- How to Increase Hemoglobin During Pregnancy? (5 Proven Ways)
- 5 Side Effects of Iron Transfusion While Pregnant (Alert)
- Is Mouth Sores Pregnancy Normal: Causes, and Safe Relief Tips
- Pregnant Heart Palpitations: What’s Normal & When to Worry?