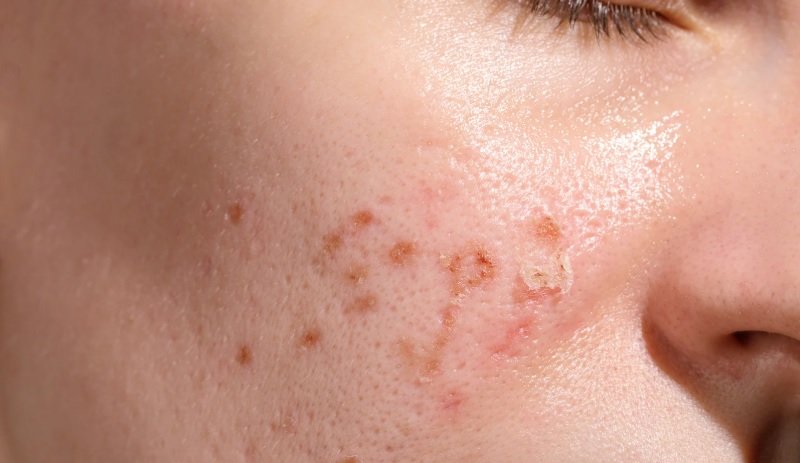
Can ADHD Meds Make Dermatillomania Worse? People with ADHD often struggle with chronic skin picking, but could their medications add fuel to the fire? If you take stimulants, do you notice more urges to pick or scratch? Is this link real, or just another misconception?
Some ADHD medications, like amphetamines or methylphenidate, may heighten anxiety or restlessness, which could trigger or worsen dermatillomania. Research suggests that while these drugs help focus, they might indirectly boost compulsive behaviors. Dr. Jon Grant, a leading expert in body-focused repetitive behaviors, highlights how managing both conditions needs a tailored plan.
If you live with attention deficit hyperactivity disorder “ADHD” and also pick at your skin, you’ll want to know how your treatment could impact you. Are there safer alternatives or strategies to keep both under control? Dive in as we explore expert insights, studies, and practical tips to manage these overlapping challenges.
Understanding Skin Picking Disorder and ADHD
Skin picking disorder SPD, also known clinically as excoriation disorder or dermatillomania, is a body-focused repetitive behavior (BFRB) characterized by recurrent picking of the skin, often leading to tissue damage, scarring, and significant distress.
Individuals with dermatillomania may pick at healthy skin, minor skin irregularities, or scabs, sometimes for hours at a time. This compulsive behavior can cause physical harm, psychological distress, and social impairment.
Dermatillomania is frequently associated with other psychiatric conditions, particularly obsessive-compulsive disorder (OCD), anxiety disorders, and attention-deficit/hyperactivity disorder (ADHD). The condition often arises as a means of coping with stress, anxiety, boredom, or uncomfortable feelings.
Many people who suffer from dermatillomania experience an intense urge to pick, followed by temporary relief but then feelings of shame or guilt afterward. Understanding the underlying psychological and neurobiological mechanisms of chronic skin picking disorder is crucial for developing effective treatment strategies.
Can ADHD Meds Make Dermatillomania Worse?
A growing number of people are asking: Can ADHD Meds Make Dermatillomania Worse? The relationship between stimulant medications commonly prescribed for ADHD — such as methylphenidate (Ritalin, Concerta) or amphetamines (Adderall, Vyvanse) — and dermatillomania is complex and worth exploring.
While these medications can significantly help individuals with ADHD manage symptoms like inattention, impulsivity, and hyperactivity, they may also inadvertently exacerbate compulsive skin picking in susceptible individuals.
There are several possible reasons why ADHD medications might worsen skin picking behavior. First, stimulant medications can sometimes increase anxiety and restlessness as side effects, which could drive a person to pick their skin as a self-soothing mechanism. Secondly, stimulants may heighten a person’s hyperfocus on minor skin imperfections, making them more prone to engage in repetitive picking.
Finally, stimulant-induced changes in dopamine regulation could potentially influence compulsive reward-seeking behavior, further complicating the management of dermatillomania.
However, it is essential to note that not everyone taking ADHD medication will experience worsening skin picking. Each individual’s response to stimulants is highly variable, and some may see improvements in their dermatillomania if their ADHD symptoms are better controlled. Ultimately, monitoring and personalized medical oversight are critical.
Managing Skin Picking Disorder and ADHD – Stimulant Medications
Balancing ADHD treatment with the management of dermatillomania can be challenging, especially when stimulant medications are involved. For patients with comorbid ADHD and Excoriation disorder, a comprehensive treatment approach is vital.
Healthcare professionals may first evaluate whether stimulant medications are truly exacerbating dermatillomania symptoms. If there is a clear correlation, options may include switching to a non-stimulant ADHD medication such as atomoxetine (Strattera) or guanfacine, which have a lower risk of triggering anxiety and compulsive behaviors.
In many cases, behavioral interventions should be added to the treatment plan. Cognitive Behavioral Therapy (CBT) has shown promise in helping patients challenge unhelpful thought patterns and develop healthier coping strategies.
Habit Reversal Training (HRT), a behavioral therapy designed for BFRBs, can also empower patients to recognize triggers and substitute skin picking with safer behaviors. Combining medication adjustments with evidence-based behavioral therapy offers the best chance of managing both ADHD and dermatillomania successfully.
It is important for patients and caregivers to communicate openly with healthcare providers if they notice a worsening of skin picking after starting ADHD medications. Tracking symptoms in a journal can help identify patterns, triggers, and the timeline of medication effects, enabling clinicians to make informed adjustments.
Table 1. Scores for depression, anxiety, impulsivity, inattention and hyperactivity questionnaires during treatment.
| Symptom | Baseline Score | After 3 Months on Stimulant Meds | After 3 Months on Non-Stimulant Meds |
|---|---|---|---|
| Depression | 18 | 20 | 15 |
| Anxiety | 16 | 22 | 14 |
| Impulsivity | 23 | 25 | 17 |
| Inattention | 28 | 14 | 16 |
| Hyperactivity | 27 | 12 | 15 |
Note: Higher scores indicate more severe symptoms. Data represent illustrative estimates for educational purposes.
Body-Focused Repetitive Behaviors: Treatments and Interventions
Body-focused repetitive behaviors like dermatillomania can be profoundly distressing, but effective treatments are available. The cornerstone of intervention is behavioral therapy, particularly cognitive behavioral therapy (CBT) and habit reversal training (HRT). These approaches teach individuals to recognize and resist the urge to pick, replacing harmful behaviors with healthier alternatives.
In addition to psychotherapy, pharmacotherapy may be considered, especially when dermatillomania co-occurs with ADHD or OCD. Selective serotonin reuptake inhibitors (SSRIs) such as fluoxetine (Prozac) or sertraline (Zoloft) may help reduce compulsive urges. N-acetylcysteine (NAC), an over-the-counter supplement, has shown promise in small studies for reducing BFRB symptoms, though more research is needed.
Support groups, whether in person or online, can also offer valuable peer encouragement and reduce feelings of shame or isolation. Apps and wearable devices that track urges or provide reminders can help build awareness and improve treatment adherence. Family education is another crucial component, as a supportive environment significantly boosts recovery odds.
Finally, practicing stress reduction techniques such as mindfulness meditation, exercise, and adequate sleep can lower baseline anxiety and reduce the triggers for compulsive skin picking. A holistic treatment strategy works best when it addresses both the biological and psychological dimensions of dermatillomania.
Commonly Asked Questions about ADHD Meds and Dermatillomania (FAQs)
Is ADHD medication bad for skin?
ADHD meds (especially stimulants) may dry skin or exacerbate picking. Stay hydrated, moisturize, and monitor changes—consult your doctor if issues persist.
Can ADHD medication make things worse?
For some, ADHD meds can worsen anxiety, insomnia, or compulsive behaviors. Adjusting dosage or switching medications with a doctor can resolve these issues.
Can ADHD meds make OCD symptoms worse?
Stimulants may intensify OCD-like behaviors (e.g., skin picking). Non-stimulant meds or CBT are alternatives—discuss symptoms with your prescriber.
How to stop compulsively picking at your skin?
Use fidget tools, cover triggers (e.g., bandaids), and practice mindfulness. CBT or NAC supplements may help—seek therapy if persistent.
What is excoriation disorder?
Excoriation disorder is compulsive skin picking causing tissue damage. Linked to OCD, it’s treated with therapy (CBT) and sometimes SSRIs. Diagnosis requires professional evaluation.
—What is dermatillomania and how is it related to ADHD?
Dermatillomania, also known as skin-picking disorder, is characterized by the compulsive urge to pick at one’s skin, often resulting in lesions and distress. Individuals with ADHD may have impulsive behaviors that can exacerbate skin-picking tendencies, creating a possible comorbidity between the two disorders.
Can ADHD medications make dermatillomania symptoms worse?
For some individuals, ADHD medications, particularly stimulants like methylphenidate, can potentially worsen skin-picking behaviors. This could be due to increased impulsivity or heightened anxiety, which might lead to compulsive skin-picking. It’s crucial to monitor symptoms closely when starting or adjusting ADHD medication.
What treatment options are available for both ADHD and skin-picking disorder?
Treatment options may include behavioral therapies such as competing response training, which helps replace the skin-picking behavior with a less harmful action. Medications used to treat ADHD, alongside cognitive-behavioral therapy for skin-picking disorder, can be effective in managing symptoms of both conditions.
How does methylphenidate treatment affect individuals with comorbid disorders?
Methylphenidate treatment in attention deficit hyperactivity may help manage ADHD symptoms but could also lead to increased anxiety or restlessness in some individuals. This heightened state may worsen behaviors associated with skin-picking or hair-pulling. A thorough evaluation by a healthcare professional is essential.
Are there any mental health disorders commonly comorbid with ADHD?
Yes, ADHD is often comorbid with various mental health disorders, including anxiety disorders, depression, and obsessive-compulsive and related disorders, such as trichotillomania and dermatillomania. These comorbidities can complicate treatment plans and require a holistic approach to management.
What are the possible mechanisms behind skin-picking in ADHD?
The possible mechanisms behind skin-picking behaviors in individuals with ADHD may include impulsivity, heightened sensory sensitivity, and difficulties with emotional regulation. These factors can lead to compulsive behaviors as a means of coping with anxiety or boredom.
How can individuals living with ADHD manage skin-picking behaviors?
Individuals living with ADHD can manage skin-picking behaviors by employing strategies such as wearing gloves or keeping hands busy with fidget toys. Engaging in mindfulness practices and seeking behavioral treatment can also help reduce the urge to pick at their skin.
Is there a link between ADHD symptoms and onychophagia (nail-biting)?
Yes, there is a potential link between ADHD symptoms and onychophagia, or nail-biting, which is another form of a compulsive behavior. Both conditions may stem from similar underlying issues such as impulsivity and anxiety, making it important to address both through comprehensive treatment.
What role does behavioral treatment play in managing ADHD and skin-picking?
Behavioral treatment plays a significant role in managing both ADHD and skin-picking disorder. Techniques like exposure and response prevention, along with cognitive-behavioral strategies, can help individuals develop healthier coping mechanisms and reduce the frequency of compulsive behaviors.
Conclusion
While stimulant medications are a mainstay of ADHD treatment, they can sometimes complicate co-occurring conditions like dermatillomania. The question — Can ADHD Meds Make Dermatillomania Worse? — does not have a one-size-fits-all answer. Some individuals may find their chronic skin picking worsens due to increased anxiety, hyperfocus, or impulsivity triggered by stimulant use, while others may see improvements if their ADHD symptoms are well controlled.
Personalized care is essential. If you or a loved one notices increased skin picking after starting ADHD medication, consult with your healthcare provider to discuss alternatives or supplemental therapies. Behavioral therapies, medication adjustments, and holistic strategies can help you achieve better management of both ADHD and dermatillomania, reducing distress and improving quality of life.
By staying informed and working collaboratively with your medical team, you can find the right balance of treatments to thrive despite these challenging co-occurring conditions.
Recommended posts
- Zoloft for ADHD Treatment: Does It Really Work or Just Hype?
- Why Does Caffeine Make People with ADHD Tired? (Hidden Facts)
- Can You Take ADHD Medication During Pregnancy? (Medical Facts)
- Do ADHD People Need More Sleep Than Others? (The Truth)