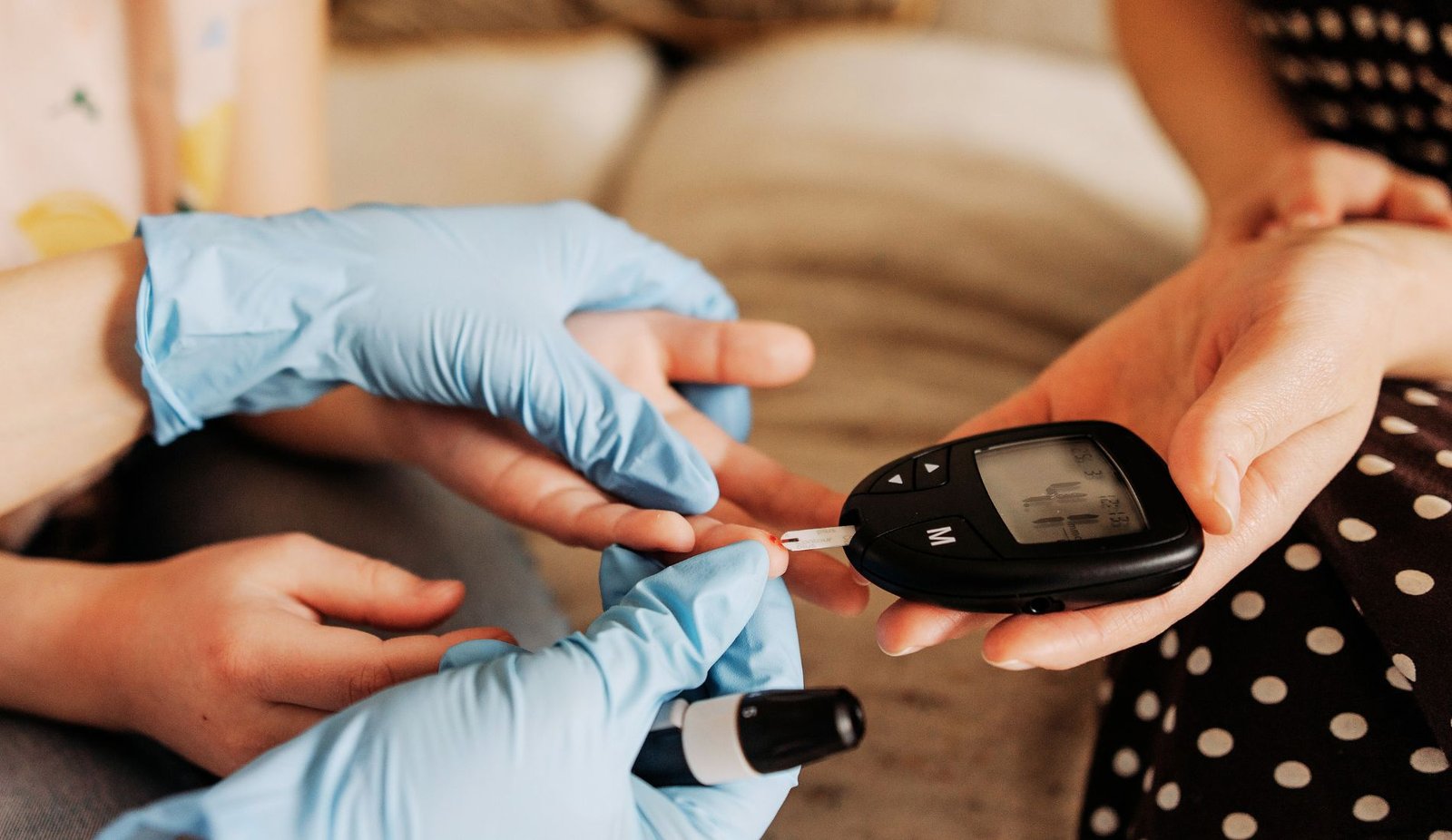
Is the medical community over diagnosing gestational diabetes, and could this trend be causing more harm than good? Over diagnosing gestational diabetes has become a growing debate among doctors and expecting mothers.
With routine screenings catching even borderline cases, many women face unnecessary stress and medical interventions during pregnancy. Research shows that some women are labeled with gestational diabetes even when their blood sugar levels pose minimal risk to them or their babies.
Leading endocrinologists like Dr. Lois Jovanovic have long argued that broadening diagnostic thresholds can inflate statistics and alter treatment patterns. This article explores the fine line between protecting maternal health and creating an epidemic of over diagnosis.
But is this expanded definition truly safeguarding mothers, or is it leading to overtreatment and fear? Renowned experts like Dr. David Simmons highlight the importance of balanced screening approaches. Let’s dive deeper into the data, expert opinions, and real-world impacts to understand whether over diagnosing gestational diabetes is a medical safeguard or a hidden burden.
Can Doctors Overdiagnosing Gestational Diabetes?
The short answer is yes, gestational diabetes mellitus overdiagnosis is possible. Medical professionals follow specific guidelines from organizations like the World Health Organization (WHO), the American Diabetes Association (ADA), and the International Association of Diabetes in Pregnancy Study Groups (IADPSG). However, these guidelines are not consistent worldwide.
Differences in diagnostic criteria—such as the glucose levels considered “abnormal”—can lead to significant variations in the number of women labeled as having gestational diabetes. For example:
- In some countries, using stricter thresholds nearly doubles the number of women diagnosed.
- A woman considered healthy in one healthcare system may be diagnosed with GDM in another.
This inconsistency raises questions about whether every diagnosis truly reflects a clinically dangerous condition or whether some women are being overtreated for borderline results.
When Does Gestational Diabetes Peak?
Gestational diabetes usually develops during the second half of pregnancy, when hormonal changes affect how the body processes glucose. The peak often occurs:
- Between 24 and 28 weeks gestation: This is when most women undergo the oral glucose tolerance test (OGTT).
- Hormonal surges in late pregnancy: Placental hormones, such as human placental lactogen, increase insulin resistance, making glucose regulation more difficult.
It is rare for gestational diabetes to appear earlier than 20 weeks, and when it does, it may indicate pre-existing undiagnosed type 2 diabetes rather than true GDM. Testing too early or repeating unnecessary tests can therefore contribute to inflated diagnosis rates.
Impact on Women with Gestational Diabetes
The impact of a gestational diabetes diagnosis can be profound. Women diagnosed with this condition often experience increased monitoring, dietary restrictions, and potential insulin therapy, which can lead to heightened stress and anxiety.
Furthermore, the psychological burden of receiving a diagnosis can affect overall maternal well-being, influencing pregnancy outcomes.
Qualitative studies have shown that women who feel overwhelmed by a gestational diabetes diagnosis may struggle with adherence to dietary and lifestyle recommendations.
This situation creates a cycle where the perceived necessity of stringent management can overshadow the actual risks posed by the condition.
Can Doctors Misdiagnose Gestational Diabetes?
Yes, misdiagnosis can occur due to several factors:
- Testing Variability: Small differences in laboratory handling or fasting compliance can influence test outcomes.
- Borderline Results: A slight deviation from the threshold may trigger a diagnosis, even if the condition would not cause complications.
- One-size-fits-all thresholds: Women of different ethnicities and body types may metabolize glucose differently, making a universal cutoff less reliable.
A misdiagnosis can subject women to months of unnecessary interventions. Conversely, underdiagnosis—failing to detect real GDM—poses its own risks, including excessive birth weight (macrosomia) and complications during delivery. The challenge lies in striking the right balance.
The Glucose Thresholds – Testing too Early
The oral glucose tolerance test (OGTT) is the standard diagnostic tool, but interpretation of thresholds is controversial. The IADPSG recommends lower cut-off points, meaning more women are classified as having GDM.
Testing too early (before 24 weeks) can:
- Capture temporary glucose fluctuations unrelated to gestational diabetes.
- Confuse pre-existing diabetes with GDM.
- Inflate diagnosis rates without evidence of improved outcomes.
For many women, repeating the test later in pregnancy provides a more accurate picture. Healthcare providers must weigh the risks of missing an early diagnosis against the consequences of unnecessary labeling.
Risks of Over Diagnosing Gestational Diabetes in Pregnancy
The risks associated with overdiagnosing gestational diabetes extend beyond immediate treatment implications. Women who receive an unnecessary diagnosis may face increased medical interventions, including induction of labor or cesarean delivery, which carry their own risks. Additionally, infants born to mothers misdiagnosed with gestational diabetes may experience unnecessary complications or interventions.
Overdiagnosis of diabetes can also lead to long-term implications, such as increased risk of type 2 diabetes in mothers and their children, as the psychological stress associated with the diagnosis can influence lifestyle choices post-pregnancy. Hence, it is crucial to strike a balance between appropriate screening and avoiding unnecessary diagnoses.
How to Cope with Gestational Diabetes Diagnosis?
For pregnant women diagnosed with gestational diabetes, coping strategies are essential to manage both physical and emotional health. Engaging with healthcare providers to understand the diagnosis and its implications is a vital first step.
Women should be encouraged to ask questions, seek support from dietitians, and participate in educational programs.
Creating a supportive network, including family and friends, can help alleviate feelings of isolation. Regular physical activity, adhering to dietary recommendations, and monitoring blood sugar levels can empower women to take control of their health. Additionally, mental health support may be beneficial for those experiencing anxiety related to their diagnosis.
Commonly Asked Questions about Overdiagnosis of Gestational Diabetes (FAQs)
Will my baby be Ok If I have gestational diabetes?
Yes, with proper management, your baby will likely be okay. Public health guidelines, informed by randomised controlled trials, show that controlling blood sugar helps prevent the condition from cause harm to your baby’s development.
What are the diagnostic criteria for gestational diabetes?
The diagnostic criteria for gestational diabetes typically include elevated blood glucose levels assessed during routine gestational diabetes screening tests. According to the new diagnostic criteria, a fasting plasma glucose level of 92 mg/dL or higher, a one-hour glucose level of 180 mg/dL or higher, or a two-hour glucose level of 153 mg/dL or higher indicates a diagnosis of gestational diabetes mellitus (GDM).
What is the importance of screening for gestational diabetes?
Screening for gestational diabetes is crucial as it helps identify women who may be at risk for hyperglycemia and adverse pregnancy outcomes. Early diagnosis allows for timely management, which can prevent complications such as neonatal hypoglycemia and large for gestational age infants.
How does gestational age affect the screening process?
Gestational age is significant in determining the timing and type of screening tests used to diagnose GDM. Typically, screening is recommended between 24 and 28 weeks of gestation, as this is when blood glucose metabolism may begin to change. Testing too early may yield false negatives, while testing too late may miss women who develop GDM later in pregnancy.
What are the potential harms of over diagnosing gestational diabetes?
Over diagnosing gestational diabetes can lead to unnecessary interventions, such as insulin injections or constant glucose monitoring, which may cause psychological stress for the mother. Moreover, it may result in increased medical costs and the risk of labeling women as having a chronic condition that could affect their future pregnancies.
Are there new criteria for diagnosing gestational diabetes?
Yes, recent updates in the diagnostic criteria for GDM indicate that slightly elevated glucose levels may not require immediate intervention. The new criteria aim to balance the risks of over diagnosis with the need for effective management, focusing on evidence of benefit from treatment.
What is the role of health services in screening for gestational diabetes?
Health services play a critical role in implementing screening for GDM and ensuring that women receive appropriate care. They are responsible for educating patients about the risks and benefits of screening and managing diagnosed cases to prevent adverse pregnancy outcomes.
How can systematic reviews inform the diagnosis of gestational diabetes?
Systematic reviews and meta-analyses provide valuable insights into the effectiveness of various screening tests and management strategies for gestational diabetes. They assess the quality of evidence regarding diagnostic criteria, helping health professionals make informed decisions about the best practices for diagnosing and managing GDM in women.
What are some challenges with the reproducibility of diagnostic tests for gestational diabetes?
Some screening tests for gestational diabetes have been criticized for poor reproducibility, meaning that results may vary significantly between tests or individuals. This inconsistency can complicate the diagnosis of GDM and may lead to unnecessary treatment or missed diagnoses in women with gestational diabetes mellitus.
What is the impact of gestational diabetes on long-term health?
Women diagnosed with gestational diabetes are at a higher risk of developing type 2 diabetes later in life. This association underscores the importance of rigorous follow-up and management of blood glucose levels after pregnancy to mitigate long-term health risks.
Conclusion
Over diagnosing gestational diabetes poses significant risks to mothers and their babies, from unnecessary medical interventions to emotional distress. By critically examining diagnostic practices and emphasizing individual patient circumstances, healthcare providers can help ensure that women receive appropriate care without the burdens of an unwarranted diagnosis. It is essential for expectant mothers to engage actively with their healthcare teams, advocating for themselves and seeking clarity to navigate this complex aspect of pregnancy effectively.
Recommended posts
- Is Gestational Diabetes Genetic from Mother or Father
- 7 Warning Signs of Gestational Diabetes You Shouldn’t Ignore
- Does Gestational Diabetes Go Away After Birth (Medical Fact)
- The Link Between Gestational Diabetes and Preeclampsia
- Is Glucose Intolerance Test in Pregnancy Optional for Moms?